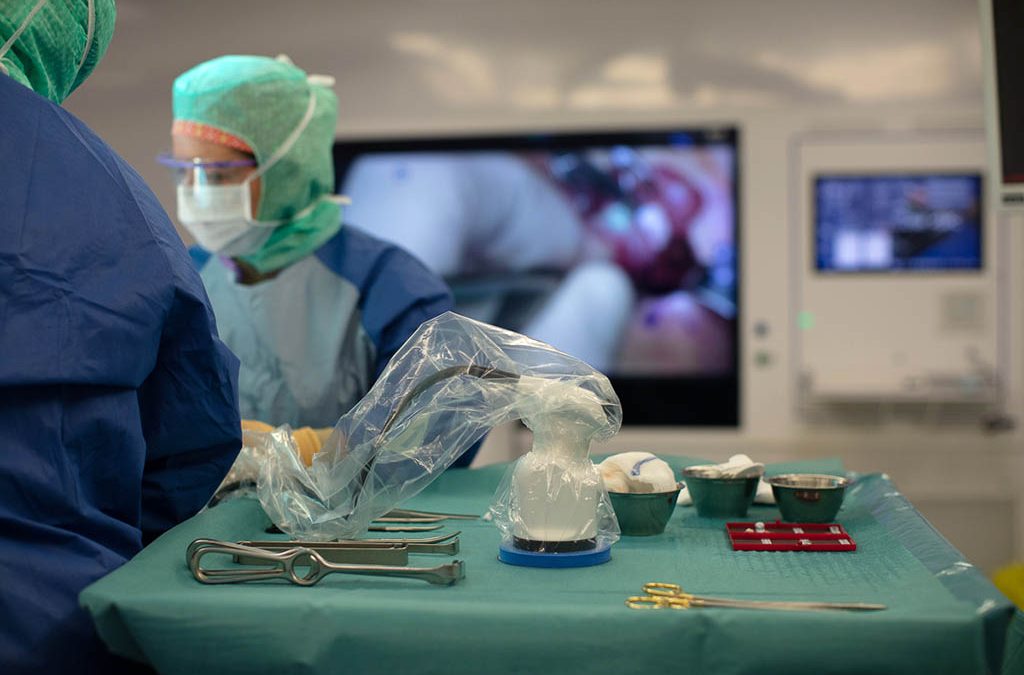
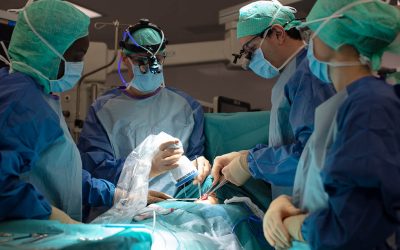
Thyroid cancer affects nearly 570,000 people worldwide every year according to the World Health Organization (WHO), 75% of whom are women. In the US, about 12,000 men and 35,000 women get thyroid cancer every year according to the Centers for Disease Control and Prevention (CDC). Thyroid cancer is characterized by the appearance of cancerous cells in the thyroid gland, forming a malignant tumor. If left untreated, these cells can migrate to other organs. This phenomenon is called metastasis. In this article, we review the different types of thyroid cancer, its prognosis, the various stages of the disease and existing treatments.
What are the different types of thyroid cancer?
- Papillary cancers are the most common, accounting for 80 to 90% of cases. These are differentiated thyroid cancers with cancerous cells retaining some of the characteristics of healthy cells.
- Follicular cancers, also called vesicular cancers, account for 10% of cases. They are also differentiated cancers. They tend to be slightly more aggressive than papillary cancers.
- Medullary cancers are rare cancers that develop from thyroid cells called C cells. They are very often familial or hereditary cancers.
- Poorly differentiated and anaplastic thyroid cancers are even rarer. They mainly affect elderly people and progress very rapidly.
Is it a serious disease?
- The age of the patient: the disease is more serious in patients over 45 years of age.
- The type of cancer: differentiated thyroid cancers (papillary and follicular cancers) are much less serious than undifferentiated cancers.
- The stage of the disease: the more or less advanced development at the time of diagnosis also influences the chances of cure.
What are the stages of thyroid cancer?
- The primary Tumor: attributing a score between 0 and 4 depending on its size and its extension to the thyroid tissue.
- Nodes: with a score between 0 and 3 depending on their number, size and extension.
- Metastasis: with a score of 0 or 1 depending on the absence or presence of metastasis.
- At stage 1, there is a single, small tumor
- At stage 2, the tumor is bigger, in a single area
- At stage 3, the cancer has extended to nearby lymph nodes
- At stage 4, the spread is wider with metastasis in other organs.
What are the treatments for thyroid cancer?
Surgical Treatment
Other Treatment
Key Figures
- 570,000 people worldwide diagnosed with thyroid cancer every year
- 75% of women
- Cure rate over 90%
Thyroid cancers are therefore cancers with high cure rates. The prognosis depends on several factors, such as the patient’s age, the type of cancer and the stage of the disease. Early diagnosis increases the chances of cure. Treatment is mainly surgical, with thyroid removal performed under general anesthesia. After the operation, hormone replacement therapy must be taken for life.