Hyperparathyroidism is a disease caused by a dysfunction of the parathyroid glands. These four small glands are located at the base of the neck, at the back of the thyroid gland. In this article, learn about hyperparathyroidism and treatment options.
What is hyperparathyroidism?
Hyperparathyroidism Causes
Hyperparathyroidism Types
There are three types of hyperparathyroidism:
- Primary hyperparathyroidism (PHPT) is a disorder of one or more of the parathyroid glands.
- Secondary hyperparathyroidism is due to the dysfunction of another organ, often the kidney, which usually affects all the parathyroid glands.
- Tertiary hyperparathyroidism can occur as a result of secondary hyperparathyroidism. The parathyroid glands develop an autonomous function.
Hyperparathyroidism Symptoms
Hyperparathyroidism Consequences
Hyperparathyroidism is also a risk factor for other diseases such as parathyroid cancer.
Hyperparathyroidism Prevalence
Hyperparathyroidism is estimated to affect 25 out of every 100,000 people. Women are twice as affected as men. The average age at diagnosis is 60.
How is hyperparathyroidism treated?
Disease Management
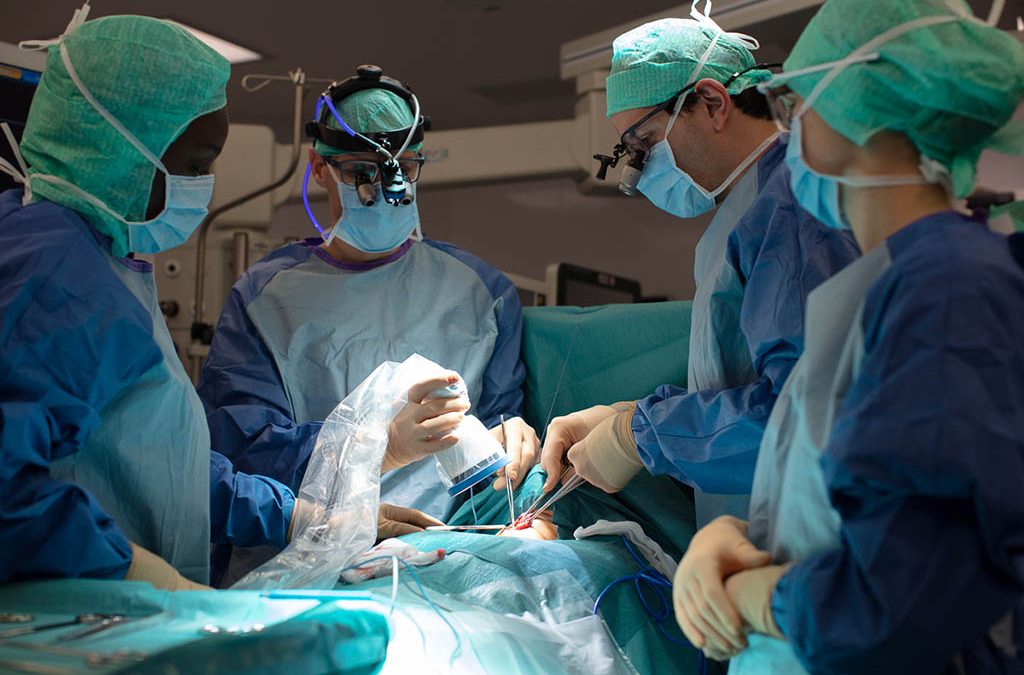
While some medications can help control hypercalcemia, treatment is mainly based on surgery. Surgery is required for primary hyperparathyroidism occurring before the age of 50 and for patients with a large number of symptoms. For secondary hyperparathyroidism, the first treatment is that of the disease causing the disorder.
Hyperparathyroidism Surgical Treatment Objectives
The surgical technique depends on the number of glands that need to be removed. If only one parathyroid gland is affected, minimally invasive surgery can be performed with an incision of 2 to 2.5 centimetres. The scar will usually be very small. If several glands are affected, then the conventional procedure has to be followed, with a larger incision to remove the glands.
Hyperparathyroidism Surgical Treatment Risks
The risks are minimized when the operation is performed by a specialized team. In addition, the use of state-of-the-art technology such as the FLUOBEAM® LX imaging solution facilitates the surgery.
Benefits of FLUOBEAM®LX for Parathyroid Surgery
“Compared to the conventional technique without imaging, the benefit is significant. […] This technique can significantly reduce postoperative hypoparathyroidism”.
Postoperative recovery
Hyperparathyroidism is therefore a disease that can have serious consequences if it is not adequately treated. Surgical treatment is effective, allowing patients to improve their quality of life. The use of innovative technologies, such as fluorescence imaging, can make it possible to minimize the risks associated with this surgical procedure.